Solving Healthcare Data Fragmentation with HIPAA-Compliant Data Platforms
- Roshy R
Introduction
A wise man once said that data isn’t the real problem. In fact, data has never been the problem; the primary challenge lies in measuring the right things and storing them in a way that makes them reusable. After all, what gets measured – gets managed.
In the healthcare industry, as in other sectors, data and its management are critical. Yet the real challenge, as we mentioned just now, is rarely the data itself. Instead, it is the ability to bring fragmented information together in a way that makes it usable, secure, and compliant.
For many healthcare organisations today, critical data exists in silos across multiple platforms. This fragmentation makes it difficult to derive real-time insights or build advanced analytics capabilities. At the same time, strict regulatory frameworks such as HIPAA introduce additional complexity around how healthcare data can be stored, accessed, and processed.
How Fragmentation Hinders Real-Time Analytics
Real-time or near-real-time data analysis has become increasingly important in healthcare. Decisions often rely on having the most current information available, whether it relates to patient care, inventory management, or operational planning.
However, fragmented systems make this difficult.
Consider a simple, very common example. Imagine a centralised database that tracks vaccine inventory across multiple locations in the U.S. Each regional store draws its inventory data from this master database. When a vaccine is purchased in one location, the inventory count should ideally be updated across the entire system immediately, so as to avoid double orders. This is the ideal situation.
Now imagine only one unit of a vaccine remains in the database. A customer purchases the last unit at a location in Virginia. If the system takes several minutes to update the central database, another location, say in Washington, may still see that unit listed as available. From the system’s perspective, the data appears correct. In reality, the vaccine has already been sold.
While this example may seem simple, it highlights a broader issue. When data updates are delayed or distributed across disconnected systems, organisations lose the ability to rely on real-time insights. Decisions are then made using information that may already be outdated.
In healthcare environments, where timing and accuracy are critical, fragmented data systems can significantly limit the effectiveness of analytics, forecasting, and operational planning.
HIPAA – Why Centralising Healthcare Data Becomes Complex
While the idea of bringing fragmented healthcare data into a centralised repository sounds straightforward, the reality is far more complicated. In regulated industries such as healthcare, centralisation introduces several technical, operational, and compliance challenges.
Security Risks of Centralised Data
A centralised healthcare data platform can become an attractive target for attackers. When sensitive patient information is aggregated into a single environment, a breach of that system could expose significantly more data than breaches affecting isolated systems. To mitigate these risks, healthcare organisations must implement strong security controls such as encryption for data both at rest and in transit, multi-factor authentication (MFA), and strict role-based access control (RBAC). Implementing and maintaining these safeguards across legacy systems and modern cloud environments is often difficult and resource-intensive.
Evolving Regulatory Requirements
The regulatory landscape surrounding healthcare data is continuously evolving. Recent HIPAA guidance and industry best practices increasingly emphasise stricter governance around cloud storage, artificial intelligence systems, and third-party data processing. This means healthcare organisations must constantly review and update their infrastructure, policies, and vendor relationships to remain compliant, often resulting in significant operational and financial overhead.
Data Standardisation and Interoperability Challenges
Centralisation also requires the integration of data from multiple heterogeneous systems. Healthcare organisations typically operate with a combination of legacy platforms, proprietary databases, and modern applications. Bringing these datasets together requires extensive data cleaning, transformation, and standardisation to align with healthcare interoperability standards such as FHIR, HL7 V2, HL7 V3/CDA, and DICOM. Additionally, organisations must reliably identify and track Protected Health Information (PHI) across systems. Without automated data governance and classification tools, this process becomes extremely complex.
Auditability and Legal Agreements
HIPAA also requires organisations to maintain detailed audit logs that record every access, modification, or deletion of PHI. These logs must be immutable, easily retrievable, and retained for extended periods, often up to six years. Furthermore, when healthcare organizations rely on external vendors or cloud platforms, they must establish Business Associate Agreements (BAAs). These agreements are often lengthy and require careful legal review, adding additional complexity to implementing centralized data platforms.
While regulatory frameworks such as HIPAA significantly influence how healthcare data can be stored, accessed, and processed, they are not the sole cause of system fragmentation. Other factors such as legacy infrastructure, vendor-specific systems, and mergers and acquisitions within the healthcare industry also contribute to the challenge of exchanging information across systems.
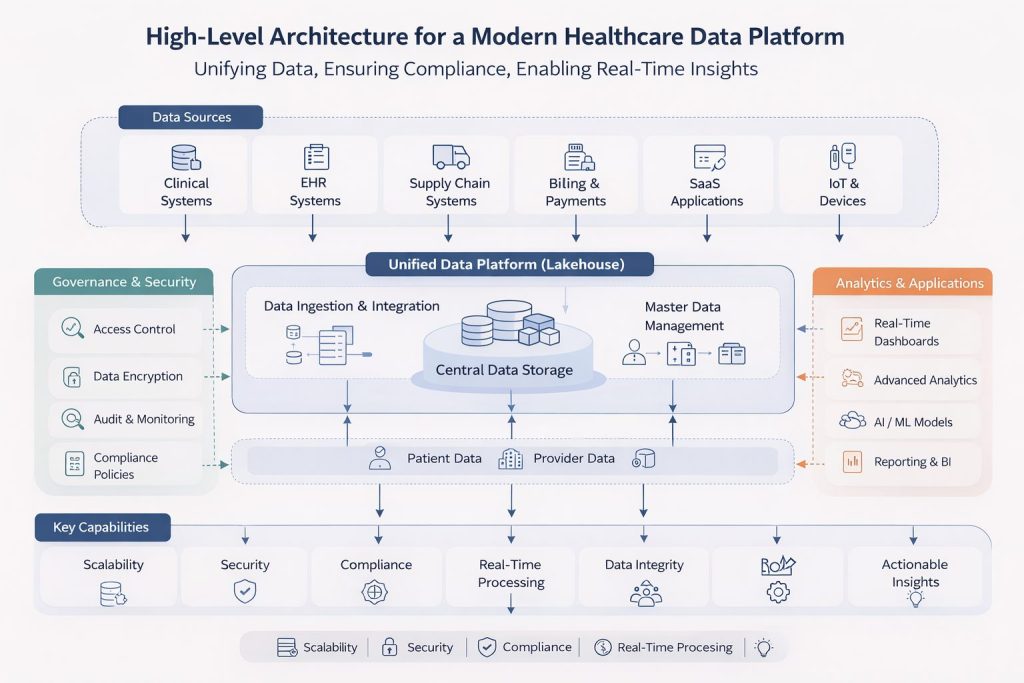
Solution: Building a Secure and Scalable Healthcare Data Platform
Regulatory frameworks within healthcare environments can always be a hard- ball to practise with, the challenges are in multiples – systems are fragmented, regulatory requirements, data security to name a few. This is why organizations are increasingly adopting modern data architectures which are designed specifically for regulated environments. The solution is not one page or one line, it is indeed multi-layered:
- Data Ingestion and Integration: Take a healthcare organisation, what might be the sources from which they are getting data from – EHR systems, clinical trial databases, supply chains, payment systems and ‘N’ no of SaaS Subscriptions. In this case, the role of a modern data pipeline is to kind of continuously ingest information from all these sources using APIs and pipelines, ensuring that the consolidation of data is done without disruption to any of the existing operations.
- Lakehouse Platforms for Unified Data Storage: Once data is ingested, it must be stored in a way that supports both scalability and governance. This is a tricky part, since many healthcare organisations are moving toward lakehouse architectures that combine the flexibility of data lakes with the structure and performance of traditional data warehouses.
- Master Data Management: Healthcare organisations often maintain multiple records for the same patient, provider, or product across different systems. In fragmented environments, the same individual may appear under multiple identities. Small variations in identifiers or demographic details can create duplicate or mislinked records. This makes it difficult to maintain a reliable enterprise view of patients, providers, or other entities.
- Governance, Security, and Access Controls: Data is sensitive; no one needs to tell that. As much as the data is important, so are the governance and access control measures relative to it. Modern data platforms, therefore, incorporate governance layers that enforce role-based access control, encryption policies, data masking, and detailed audit logging.
Source: Digital Transformation Demands an Accurate Trusted Identity Data, Healthcare IT News
Building Healthcare Data Platforms for the Future
Designing and implementing such data platforms requires deep expertise across data engineering, governance frameworks, and regulatory compliance.
At Innovature, we work with organisations to design scalable data platforms that integrate fragmented systems, support advanced analytics, and maintain strict compliance with regulatory frameworks such as HIPAA.
By combining modern data engineering practices with strong governance models, organisations can unlock the full value of their healthcare data while ensuring security, reliability, and regulatory alignment.
Conclusion
Healthcare organisations today generate enormous volumes of data across clinical systems, operational platforms, and supply chain networks. However, the real challenge lies not in collecting this data but in transforming it into reliable, secure, and actionable insights.
Fragmented systems, evolving regulatory frameworks, and complex governance requirements make this task difficult. Modern data architectures that integrate secure data pipelines, unified storage platforms, master data management, and governance frameworks provide a path forward.
By adopting such architectures, healthcare organisations can move toward real-time analytics while maintaining the compliance and security standards required in regulated environments.










